
How can I know?
Do you suffer from arthritis or osteoarthritis? It’s time to get the facts straight.
First, it’s important to mention that these are two different conditions, even though osteoarthritis is a form of arthritis—and certainly the most common one.
Arthritis is an umbrella term that encompasses more than 100 different joint diseases that all differ in terms of their intensity, location, age of onset, symptoms, etc.
Osteoarthritis
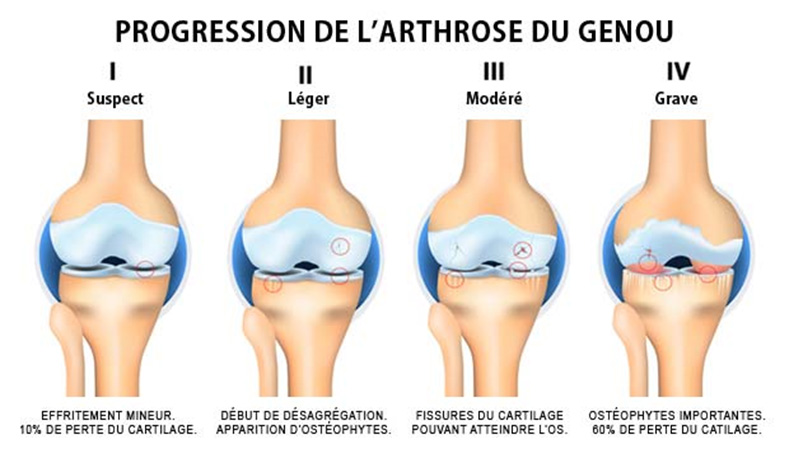
Osteoarthritis affects more Canadians than all other forms of arthritis combined—roughly 1 in 6 people, according to the Arthritis Society. The Osteoarthritis Research Society International describes it as “the body’s failed attempt to repair damaged joint tissues.” Cartilage, the rubbery substance at the end of your bones, gradually deteriorates with age or following an injury. Your weight also plays a major role in the progression of this disease, along with your occupation and any pre-existing joint deformities. There are 4 stages of osteoarthritis:
- Minor: Some minor degenerative changes in the bones (normally without pain).
- Mild: More noticeable bone spurs and erosion of the cartilage (like a floor that’s become scuffed and slightly warped from daily wear and tear).
- Moderate: Tears in the cartilage (the floor is cracked but still functional).
- Severe: Cartilage almost completely gone in places, bones rubbing against each other (there are holes in the floor, making it hard to walk on).
(Image source: https://www.santeplusmag.com/le-moyen-le-plus-simple-pour-prevenir-larthrose/_ )
Arthritis
The other forms of inflammatory arthritis are mostly what are known as “autoimmune diseases,” where the body attacks normal, healthy tissues as though they were invaders. Inflammatory reactions normally occur as flare-ups, causing damage at a much faster rate than osteoarthritis. The most common forms are juvenile arthritis, rheumatoid arthritis, ankylosing spondylitis, psoriatic arthritis, and gout, to name a few.
Here’s a (non-exhaustive) table that sums up the main differences:
| Arthritis | Osteoarthritis | |
| Diagnosis | Based on symptoms, family history (genetics), imaging tests, and blood tests | Based on symptoms and x-rays |
| Schedule | Pain at night | Pain during the day |
| Morning stiffness | Souvent plus de 1 heure | 30 minutes or less |
| Pain |
|
|
| Location | Inflammation of one or more joints, depending on the type of arthritis | Very gradual onset in joints that bear the most stress (knee, hip, spine, hand) |
| Symptoms | Pain, joint stiffness, joint swelling (potentially rapid and severe), heat, redness in the affected area, relatively rapid joint deformities (over a few years), loss of range of motion, systemic symptoms (fever, digestive problems, etc.) | Pain, morning stiffness, very gradual joint deformities (over many years), joint cracking during specific movements, loss of range of motion over time, long-term loss of mobility |
| Age of onset | Varies depending on the type of arthritis (forms affecting children, adults, and seniors) | Gradual onset with age |
| Treatments |
|
|
In both cases, your doctor and health professional (physiotherapist, osteopath, etc.) can help you slow the progression of the condition and maintain a good quality of life. That being said, once damage has already occurred, it’s not usually reversible.
To help you raise the issue with your doctor or health professional, you can answer the 6 questions in this symptom checker: https://arthritis.ca/about-arthritis/signs-of-arthritis/symptom-checker/.
So, is it arthritis or osteoarthritis?
Sources :
- Arthritis Society website: https://arthritis.ca/
- 2. Excellent (and very entertaining) column by Le Pharmachien on the subject (in french only): http://lepharmachien.com/arthrite-arthrose/
Need to talk to a professional?
Other articles that might interest you...

Walking: 4 powerful benefits for osteoarthritis
The perfect exercise Did your doctor recently tell you that your joint pain may be caused by...

What is occupational therapy in mental health?
Understanding this approach Occupational therapy is for people who have trouble performing their...
My shoulder hurts. What should I do?
Rotator cuff tendinopathy Rotator cuff tendinopathy usually presents as shoulder pain that can...
 Home
Home